15 Years to Be Believed: Marissa Furey’s Fight for a Diagnosis of Behçet’s Disease

Marissa lives in West Greenwich, Rhode Island, where daily life now feels both hard-won and deeply appreciated—something she once could not take for granted. At 39, she reflected on a journey that has reshaped nearly every part of her life—from her career in molecular biology to something as simple as a walk on the beach.
Before illness, Marissa described herself as detail-oriented, organized, and driven, with a sarcastic edge and a stubborn streak that served her well in a demanding scientific field. She worked as a research specialist in transgenics, genomics, and microbiology. Today, those traits have shifted. She now experiences neurological flare-ups that affect attention, memory, and executive functioning, often feeling scattered and unable to follow directions as she once could. Yet alongside those losses, something else has emerged. “I have become more thankful for family, travel and small everyday tasks.”
Her life is anchored by her husband of 14 years, Christopher—a family medicine physician—and their 10-year-old daughter. Despite everything, Marissa still finds joy in music, playing piano in two bands and performing at open mics. She exercises with a trainer, explores hobbies like pickleball, and treasures time playing video games with her daughter. “Always looking to try something new if I am able,” she said. But the road to her current stability has been long, complex, and often traumatic.
Early Symptoms, No Answers
Marissa’s symptoms began in childhood. At age 10, she experienced a severe migraine with visual and sensory aura that caused partial vision loss and numbness. By 15, she had vertigo and fainting episodes, diagnosed as Meniere’s disease. In her early 20s, new symptoms emerged: canker sores, joint swelling, and severe cystic acne. Still, no unifying diagnosis was made.
At 25, she woke up with what she described as a giant black spot in her left eye. She began seeing more floaters and had hazy, smoky vision. Months later, she was diagnosed with intermediate uveitis and retinal vasculitis (both eyes). This form of uveitis is associated with several autoimmune conditions, including multiple sclerosis [MS], sarcoidosis, Behçet’s disease, and lupus. Around the same time, doctors considered MS after finding a brain lesion and a genetic marker (HLADR15) but chose to monitor rather than treat—an early example of a pattern that would repeat for years.
Marissa’s uveitis specialist, ophthalmologist Dr. Stephen Anesi, worked for many years during this time to try to treat the uveitis as well as the systemic condition he believed to be underlying with multiple immunosuppressant treatments that failed or caused severe side effects. He placed a steroid eye implant and treated glaucoma with laser surgery. He recommended that Marissa see other specialists and continued to advocate for a broader workup, concerned there was an underlying systemic inflammatory or vasculitic process—though these efforts often did not bring her closer to a diagnosis.
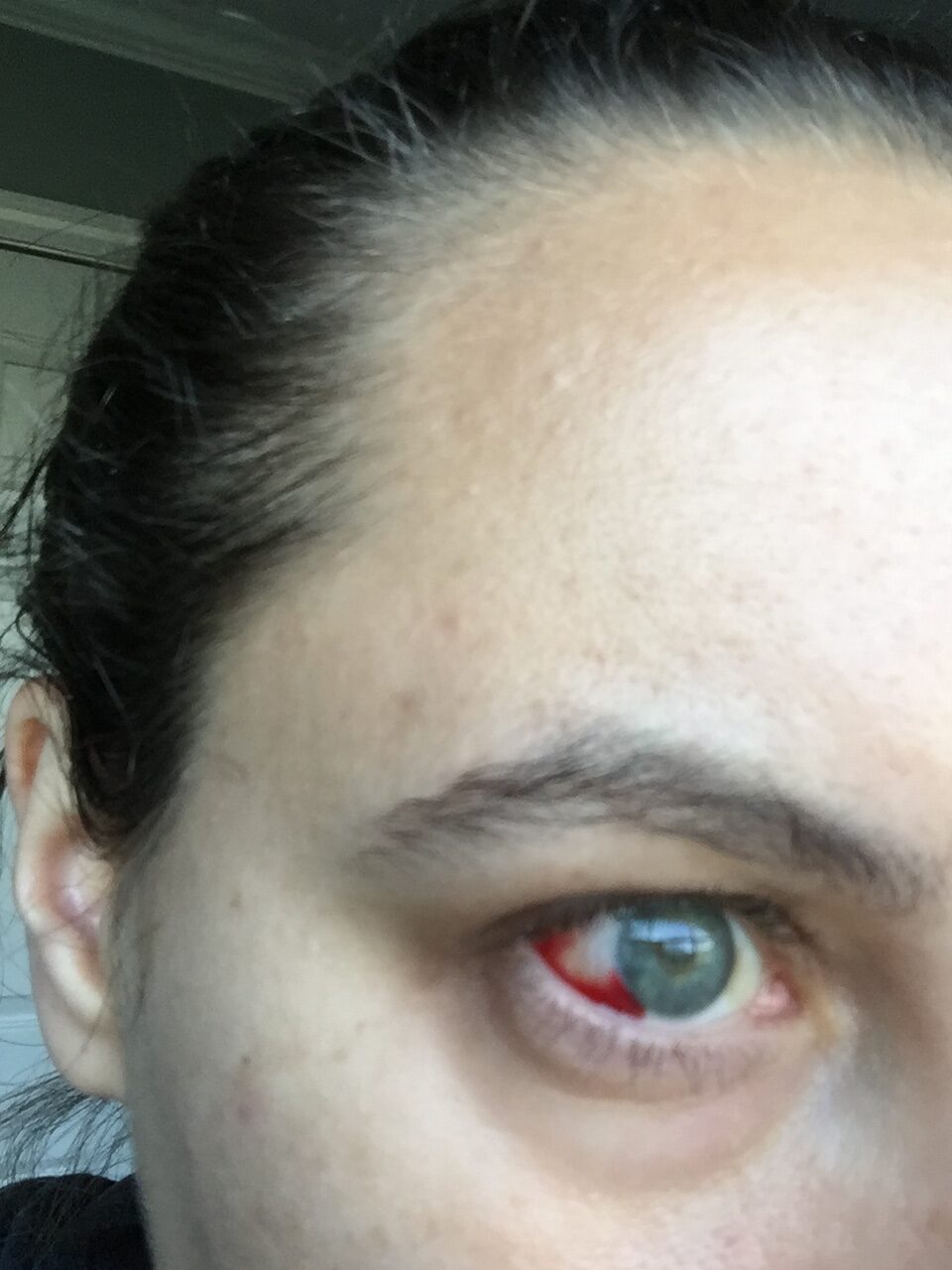
Years of Misdiagnosis and Dismissal
During her pregnancy at 28, Marissa experienced stroke-like neurological symptoms. She woke up one day repeating the same word, her left arm was completely numb, she had confusion, an inability to speak, and tremors. Imaging again revealed brain lesions. “My husband was terrified and brought me to the ER. After the brain MRI, they said it looked like MS and asked me if I had a neurologist.” She continued seeing the same neurologist for over a decade and trusted his judgment at the time. Looking back, her feelings are stark: “I feel betrayed… just because he thought it’s not MS does not mean you do absolutely nothing—no exploration of other diagnoses, no treatment, no referral.”
Over the next decade, her condition escalated. She developed heart palpitations and arrhythmia (had to have a heart ablation), hearing loss that now requires hearing aids (in her 30s), recurrent eye inflammation (panuveitis/vasculitis flares) and arthritis in multiple joints. She cycled through immunosuppressants, many of which either failed or caused severe side effects. Some treatment options were also limited by diagnostic uncertainty—for example, therapies like Remicade® are typically avoided when MS is suspected, further complicating decisions about her care. Steroids consistently helped—but only temporarily.
By her early 30s, her health had become a maze of overlapping conditions: probable posterior scleritis, postural orthostatic tachycardia syndrome (POTS), small fiber neuropathy, recurring infections, and widespread inflammation. Multiple diseases were considered—lupus, sarcoidosis, and Susac’s syndrome. Cogan’s syndrome was also proposed by a different neurologist, but no one fully explained the entire picture and not everyone agreed. Then came more neurological episodes.
In 2022, she was hospitalized with severe stroke-like symptoms: facial drooping, loss of speech, weakness, problems walking, confusion, fever, and tremors all over her body. A “code stroke” was called—but it wasn’t a stroke. Testing showed abnormalities in her cerebrospinal fluid and EEG, yet her symptoms were attributed to hemiplegic migraine or functional neurological disorder. “I had to beg to have CSF (cerebrospinal) testing done,” she said. These episodes became recurring—and increasingly difficult to be taken seriously.
Later that year, Marissa received a diagnosis of Behçet’s disease at a specialty clinic, based on a constellation of symptoms including oral ulcers, eye inflammation, arthritis, and skin findings. However, her neurological symptoms were still not fully recognized as part of the same disease process. “They were completely dismissed… as ‘migraine,’” she said.
The following years brought repeated hospitalizations, worsening neurological attacks, severe headaches and eye pain, and mounting frustration. After one visit, she recalled being discharged unable to walk correctly after being “lectured” about stress and told to seek psychological care.
“Again, Dr. Anesi tried to help, seeing how horrible my condition had become,” Marissa explained. “My husband brought me in, and I couldn’t speak correctly or walk at an office appointment. Dr. Anesi prescribed high-dose IV Solu-Medrol® (corticosteroid), which always helped temporarily but would keep wearing off.” The doctor was concerned this was Neuro Behçet’s disease or some type of inflammatory vasculitis, reinforcing a long-standing concern that her symptoms were driven by an underlying systemic inflammatory or vasculitic process.
At one point, a neurology resident physician told her to try ketamine and “trip balls”—a moment she described as both shocking and symbolic of how misunderstood her condition had become.
Despite exhaustive migraine treatments—medications, Botox®, nerve blocks—nothing worked. Eventually, Marissa established care with a neurologist specializing in headaches, Dr. Roderick Spears. He tried many medications to help with her symptoms but quickly concluded that they were not the result of a migraine. He suggested getting another evaluation at the Cleveland Clinic. “I want to thank Dr. Spears for his efforts in trying to treat this and manage the symptoms with effective pain medications in an attempt to keep me out of the hospital,” Marissa said.
By 2024, at the Cleveland Clinic, specialists agreed her condition was likely a form of vasculitis, possibly related to Behçet’s disease, and emphasized the need for aggressive treatment. She began Rituxan® infusions but remained dependent on steroids.

2025: A Turning Point in Treatment
After years of trial and error, Dr. Anesi prescribed Cortrophin® gel. Around that time, Marissa developed a new eye movement problem—double vision—and couldn’t look all the way up with her left eye, a condition known as Brown syndrome (eye muscle inflammation). She has not experienced these symptoms since starting the medication.
“THIS WAS LIFE CHANGING,” Marissa said. “My eyes are completely normal. My eye symptoms and chronic head pain are gone, stroke-like symptoms are minimal, and even my POTS/heart symptoms have improved, along with arthritis, fatigue, and canker sores. I feel better than I have in about five years.”
“I also credit my rheumatologist, Dr. Eli Miloslavsky, for ordering Remicade infusions and never dismissing any of my symptoms over the years and his willingness to treat this confusion regardless of the name or label for it,” Marissa said. “Remicade has also been a great addition to treatment for the past year. My health has continued to improve, and I hope to eventually come off steroid-based medication.”
Today, she continues treatment with Cortrophin, Remicade infusions, and methotrexate. While not without side effects, the regimen has allowed her to taper off steroids and regain parts of her life. She has not been hospitalized in over a year and believes she may be approaching remission.
Still, the impact of the disease lingers. Marissa lives with tremors, hearing loss, intermittent confusion, and the unpredictability of flare-ups. Her career in molecular biology has been derailed. “It has affected everything,” she said, from daily functioning to her ability to be present with her family.
Emotionally, the toll has been just as significant. “It’s made me very angry with the medical system (specifically neurology),” she admitted. Yet she also described a shift in perspective. “It has also made me appreciate small things like taking a walk… and being able to go on vacation.”
Marissa’s diagnosis—now considered Neuro-Behçet’s disease, or Behçet’s with neurological involvement—took more than 15 years. Even now, some physicians hesitate to fully commit to the label, reflecting the uncertainty that still surrounds her case. “They are not 100 percent,” she said.
Moving Forward
What sustained her through it all was persistence. Marissa became her own advocate, organizing medical records, researching diagnostic criteria, and pushing for testing. “Don’t assume your specialist has reviewed anything,” she advised. “Bring the information and results to them directly.”
“I have also raised more than $5,000 since 2018, participating in Boston’s Ocular Immunology and Uveitis Foundation Walk for Vision 5K with my family. I was their patient speaker in 2024.”
She also found strength in connection—family, friends, music, and conversations with others facing similar struggles. At the same time, those conversations revealed a troubling pattern. “I could make a list of people diagnosed with Behçet’s disease… told they are ‘stressed, it’s migraine, it’s FND (functional neurological disorder),’” Marissa said. “It’s really heartbreaking and disappointing that good people with families are dismissed and not getting access to life-changing treatment.”
Looking ahead, her hope is simple: progress through awareness and research. “Physicians need to continue to have curiosity… just because it is rare does not mean it doesn’t exist.”
If there is one message she hopes others take away, it’s this: “Think about if it were yourself… no one asked for this.” And for those still searching for answers: “Don’t give up. Advocate for yourself. Push for answers and treatment no matter what is said to you. It’s your health and your life.”
Marissa added, “Physicians, please believe your patients. One day you might become one.” She shared her story with the hope that specialists and hospitalists will read this, and something will change. For her, the main issues were breakdowns in doctor-patient interactions, poor communication between specialties, bias, and inadequate testing—patterns she believes continue to affect others seeking answers.
